|
The long-term management in congenital Long QT syndrome is with beta-blockers as help prevent ventricular arrhythmias by stabilizing ventricular action potential and helping block sympathetic surges associated with arrhythmias. The goal of management is the prevention of lethal arrhythmias such as torsade de pointes (TdP). It is important to refer these patients to the cardiologist/cardiac surgeon ASAP as the management is complex. Patients with a prolonged QT interval may be first identified by the primary care provider, nurse practitioner, internist or pharmacist. It also may be indicated in asymptomatic individuals who are suspected to be at high risk for ventricular arrhythmias. It is also indicated in those whom have beta-blocker resistant symptoms or have contraindications to beta-blockers. An implantable cardioverter defibrillator (ICD) is recommended in patients with Long QT syndrome who were resuscitated from a cardiac arrest. įor long-term management in congenital Long QT syndrome, beta-blockers are the first line choice, and they help prevent ventricular arrhythmias by stabilizing ventricular action potential and helping block sympathetic surges associated with arrhythmias. In those who do not respond to magnesium sulfate, temporary transvenous overdrive pacing should be considered. Isoproterenol and Class IB antiarrhythmic drugs, such as lidocaine and phenytoin may also be used. Also, first-line treatment is magnesium sulfate, and the benefit is seen independent of serum magnesium level. A patient who is hemodynamically unstable should receive non-synchronized electrical defibrillation. As described earlier, the longer the QT interval, the higher the risk is for torsade de pointes. 
In patients with LQT2, there is marked shortening with exercise, however, exaggerated lengthening of the QT interval as the heart rate declines during late recovery. 
Their ECG shows the failure of the QT interval to shorten with increased heart rates, or it may even show prolongation. The concept of this testing is that patients with Long QT syndrome have an abnormal response to sympathetic stimulation. 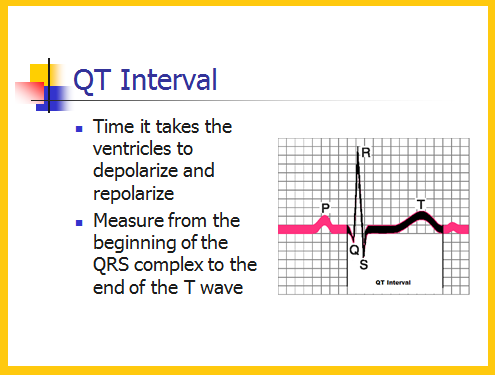
Pharmacologic provocation with epinephrine or isoproterenol is warranted in patients with a borderline presentation. Genetic testing of the patient and family members is the gold standard however, this testing is limited by cost. Noncardiac phenotype (as discussed above) may aid in making the diagnosis. In those patients, it may be very helpful to obtain an electrocardiography of the patient and family members. In the absence of reversible or acquired causes of QT prolongation, the diagnosis of Long QT syndrome is made. Also, stimulating thyroid hormone (TSH) levels may be checked in patients with suspected hypothyroidism. The most common cause of QT prolongation in an ICU setting is usually drug-related. Serum potassium, calcium, and magnesium levels should be checked, as low serum of each can cause QT prolongation. 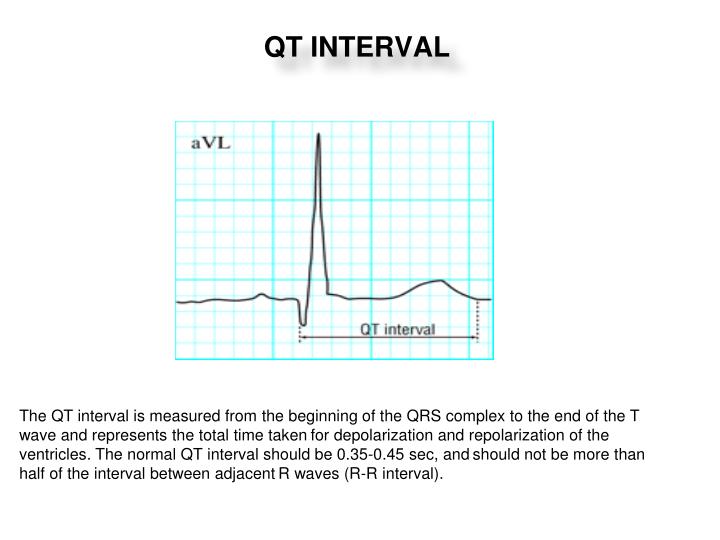
Once QTc is identified as prolonged, the next step in a workup is to look for acquired causes. Though Bazett formula seems to be relatively accurate in heart rates between 60 to 100 beats/min, it tends to overcorrect with higher heart rates and undercorrect in lower heart rates. While several equations exist to help correct for variation in heart rate, the most commonly used is Bazett formula ( QTC = QT / √ RR ). A QTc greater than 500 is associated with increased risk of torsade de pointes. This is known as QTc. QTc is prolonged if it is greater than 440 ms in men or greater than 460 ms in women. ĭue to the variation of QT interval with heart rate (higher heart rate has shorter QT interval, lower heart rate has longer QT interval), it is important to correct the QT interval for the heart rate. A helpful tip that helps identify prolonged QT interval on initial examination of the ECG is that a normal QT interval should be less than half the preceding RR interval. On the contrary, if the U wave is small or separate from the T-wave then it should be excluded. The maximum slope-intercept method is used to define the end of the T wave. If a U wave exists and is large (greater than 1 mm), and fused with T-wave, then this should be included in the QT measurement. This should be done on several successive beats, of which the longest interval is chosen. This is often done on lead II or V5-6, whichever is longer. Establishing the diagnosis of prolonged QT starts by measuring the QT interval on ECG.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
